Onychomycosis is the most common nail disease.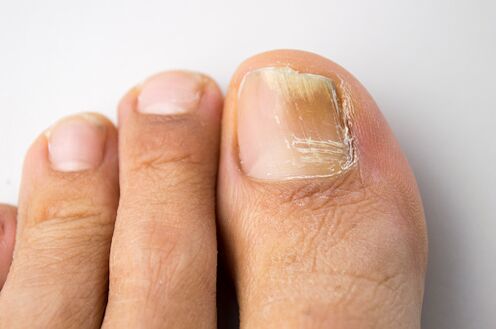 It was found that 50% of cases of changes in the nail plates are related to mycotic infection.Epidemiological studies conducted in Russia and foreign countries revealed a high frequency of onychomycosis, which ranged from 2 to 13% in the general population.The risk of developing onychomycosis is highest in elderly patients.For example, in people over 70 years of age, the prevalence of onychomycosis of the feet can be 50% or more.It is believed that the slow growth of the nail plates, disorders of the peripheral and main circulation in the elderly contribute to this.A high incidence of onychomycosis has also been found in patients with immunodeficiency conditions (including AIDS patients) and in patients with diabetes mellitus.
It was found that 50% of cases of changes in the nail plates are related to mycotic infection.Epidemiological studies conducted in Russia and foreign countries revealed a high frequency of onychomycosis, which ranged from 2 to 13% in the general population.The risk of developing onychomycosis is highest in elderly patients.For example, in people over 70 years of age, the prevalence of onychomycosis of the feet can be 50% or more.It is believed that the slow growth of the nail plates, disorders of the peripheral and main circulation in the elderly contribute to this.A high incidence of onychomycosis has also been found in patients with immunodeficiency conditions (including AIDS patients) and in patients with diabetes mellitus.
Often, patients and some doctors perceive onychomycosis as an exclusively aesthetic problem.However, this is a serious disease that occurs chronically and in cases of immunodeficiency or decompensation of endocrine diseases can cause the development of widespread mycosis of the skin and its appendages.Onychomycosis is often accompanied by the development of severe complications, such as diabetic foot, chronic erysipelas of the extremities, lymphostasis and elephantiasis.In patients receiving cytostatic or immunosuppressive therapy, the disease can cause the development of invasive mycoses.That is why onychomycosis treatment is necessary and should be carried out on time.
Only a few decades ago, the treatment of onychomycosis was labor-intensive, time-consuming and unpromising.Medicines used in the treatment of fungal diseases of the skin and its appendages are characterized by low effectiveness and high toxicity.Achieving a positive result required long-term treatment or an increase in the dosage of drugs, which was often accompanied by severe complications.Some treatments were potentially life-threatening to patients.For example, X-ray therapy, the use of thallium and mercury led to the development of skin cancer, diseases of the brain and internal organs in patients.
The emergence of highly effective and low-toxic antifungal drugs has greatly facilitated the treatment of fungal diseases of the skin and its appendages.However, the results of the application of new antimycotics were not satisfactory.Controlled clinical trials have shown that the effectiveness of systemic antimycotics after treatment is from 40 to 80%, and after 5 years - from 14 to 50%.At the same time, the effectiveness of onychomycosis therapy increases with the use of complex treatment methods, which include the use of etiotropic drugs and agents that affect pathogenesis.Also, as a result of clinical trials conducted in European countries, it was determined that the effectiveness of onychomycosis treatment can be increased by an average of 15% with the combined use of systemic antimycotics and antifungal varnishes containing amorolfine.
Treatment
For the treatment of onychomycosis, drugs are used that differ in their chemical composition, mechanism of action, pharmacokinetics and spectrum of antifungal activity.A common property for them is a specific effect on pathogenic fungi.This group consists of azoles (itraconazole, fluconazole, ketoconazole), allylamines (terbinafine, naftifine), griseofulvin, amorolfine, ciclopirox.For the treatment of onychomycosis, systemic drugs belonging to the azole group - itraconazole, fluconazole, as well as the allylamine group - terbinafine are used.Griseofulvin and ketoconazole are not currently prescribed for the treatment of onychomycosis due to low efficacy and high risk of adverse events.Lacquers and solutions containing amorolfine and ciclopirox are used as external agents for onychomycosis.
Allilaminesare synthetic antifungals.Allylamines primarily act on dermatomycetes, while they have a fungicidal effect.The mechanism of their action is the inhibition of the enzyme squalene epoxidase, which participates in the synthesis of ergosterol, the main structural component of the cell membrane of dermatomycetes.Allylamines include terbinafine and naftifine.
Allylamines are active against most dermatomycetes (Epidermophyton spp., Trichophyton spp., Microsporum spp., Malassezia spp.), the causative agent of chromomycosis and some other fungi.
Indications for oral use of terbinafine are onychomycosis, common forms of dermatomycosis of the skin, mycosis of the scalp, chromomycosis.Indications for external use of terbinafine and naftifine include limited skin lesions due to mycosis, pityriasis versicolor and cutaneous candidiasis.Terbinafine has high bioavailability and is well absorbed from the gastrointestinal tract regardless of food intake.In high concentrations, the drug accumulates in the stratum corneum of the skin, nail plates, hair, and is excreted with the secretions of the sweat and sebaceous glands.Absorption of terbinafine when applied locally is less than 5%, naftifine - 4-6%.The concentration of terbinafine and naftifine in the skin and its appendages significantly exceeds the MIC for the main pathogens of dermatomycosis.Correction of the dosage regimen of terbinafine may be necessary in combination with inducers (rifampicin) or inhibitors of microsomal liver enzymes (cimetidine), since the former increase its clearance, and the latter decrease it.
As a result of numerous controlled multicenter comparative clinical trials, it was established that terbinafine is the most effective antifungal agent in the treatment of onychomycosis.
Terbinafineused for widespread skin lesions, onychomycosis, chromomycosis, in such cases terbinafine is prescribed orally.Terbinafine is the drug of choice in the treatment of onychomycosis, because it is the most effective against the main causative agents of onychomycosis - dermatomycetes.Contraindications for the use of allylamine are allergic reactions to drugs of the allylamine group, pregnancy, breastfeeding, age under 2 years, liver diseases accompanied by impaired liver function (increased transaminases).
Azoles- the largest group of synthetic antimycotics.In 1984, the first systemic antifungal drug from the azole group, ketoconazole, was introduced into practice, in 1990, fluconazole, and in 1992, itraconazole.
Azoles used as systemic drugs have a predominantly fungistatic effect.An important advantage of azoles compared to other drugs is their broad spectrum of antifungal activity.Itraconazole is active in vitro against most of the causative agents of onychomycosis - dermatomycetes (Epidermophyton spp., Trichophyton spp., Microsporum spp.), Candida spp.(C. albicans, C. parapsilosis, C. tropicalis, C. lusitaniae, etc.), Aspergillus spp., Fusarium spp., S. Shenckii, etc.Fluconazole is active against dermatomycetes (Epidermophyton spp., Trichophyton spp.) and Microsporum spp.(C. albicans, C. parapsilosis, C. tropicalis, C. lusitaniae, etc.), but does not affect Aspergillus spp., Scopulariopsis spp., Scedosporium spp.
The pharmacokinetics of different azoles are different.Fluconazole (90%) is well absorbed from the gastrointestinal tract.A normal level of acidity is necessary for good absorption of itraconazole.If the patient taking these drugs has low acidity, their absorption decreases and, consequently, their bioavailability decreases.Absorption of itraconazole solution is higher than in itraconazole capsules.Itraconazole capsules should be taken with food, and itraconazole solution on an empty stomach.
Itraconazole is metabolized in the liver and excreted from the body through the gastrointestinal tract.It is also secreted in small amounts by sebaceous and sweat glands.Fluconazole is partially metabolized and mostly excreted unchanged by the kidneys (80%).
Itraconazole interacts with many medications.The bioavailability of ketoconazole and itraconazole is reduced when taking antacids, anticholinergics, H2 blockers, proton pump inhibitors and didanosine.Itraconazole is an active cytochrome P450 isoenzyme inhibitor and can alter the metabolism of many drugs.Fluconazole affects the metabolism of drugs to a lesser extent.It is unacceptable to take azoles with terfenadine, astemizole, cisapride, quinidine, because fatal ventricular arrhythmias can develop.Simultaneous use of azoles and oral antidiabetics requires constant monitoring of blood glucose levels, as hypoglycemia may develop.Taking indirect anticoagulants of the coumarin and azole group may be accompanied by hypocoagulation and bleeding;therefore, hemostasis control is necessary.Itraconazole can increase the concentration of cyclosporine and digoxin in the blood, and fluconazole - theophylline and cause the development of a toxic effect.It is necessary to adjust the dose and constantly monitor the concentration of the drug in the blood.The combined use of itraconazole with lovastatin, simvastatin, rifampicin, isoniazid, carbamazepine, cimetidine, clarithromycin, erythromycin is contraindicated.Fluconazole should not be used with isoniazid and terfenadine.
Itraconazoleit is used for dermatomycosis (athlete's foot, trichophytosis, microsporia), pityriasis versicolor, candidiasis of the skin, nails and mucous membranes, esophagus, vulvovaginal candidiasis, cryptococcosis, aspergillosis, pheotrichosis for endohyphomycosis, chromohyphomycosis, prevention of mycosis in AIDS.
Fluconazoleit is used for the treatment of generalized candidiasis, all forms of invasive candidiasis, including immunocompromised patients, genital candidiasis, candidiasis of the skin, its appendages and mucous membranes.Recently, due to its safety and good tolerability, fluconazole is increasingly used to treat patients with dermatomycosis with damage to the skin and its appendages (nails and hair).
Amorolfineit is included in a varnish used to treat onychomycosis.The mechanism of action of amorolfine is to disrupt the synthesis of ergosterol, the main component of the cell membrane of the fungus.It has a fungistatic and fungicidal effect.It has a wide spectrum of action.The concentration of amorolfine in the nail plate significantly exceeds the MIC for the main pathogenic dermatomycoses for 7 days.Therefore, the drug can be applied no more than 1-2 times a week, which makes its use economically profitable.Contraindications: allergic reactions to amorolfine, infants and small children.Varnish as monotherapy is prescribed when no more than 1-3 nail plates are affected and no more than 1/2 of the surface from the distal end.Amorolfine can also be used in combination with systemic antifungals for more widespread nail damage.
Ciclopiroxhas a fungistatic effect.Active against dermatomycetes, yeast-like fungi and filamentous fungi, molds, as well as some gram-negative and gram-positive bacteria.Ciclopirox (varnish) is used as monotherapy when a maximum of 1-3 nail plates are affected, not more than 1/2 of the surface from the distal end.Ciclopirox can also be used in combination with systemic antifungals for more widespread nail damage.Contraindications: allergic reactions to ciclopirox, infants and early childhood, pregnancy and breastfeeding.
List of recommended laboratory tests when prescribing systemic antifungal drugs.
- Clinical blood test.
- General urinalysis.
- Biochemical blood test (ALT, AST, bilirubin, creatinine).
- Ultrasound of abdominal organs and kidneys (preferred).
- Pregnancy test (preferred).
Treatment of basic diseases.The effectiveness of the use of antimycotics increases with the correction of pathological conditions that contribute to the development of onychomycosis.Before starting antimycotic therapy in patients with somatic, endocrine, neurological diseases and circulatory disorders in the extremities, it is necessary to conduct an examination to determine the main symptom complex that contributed to the development of dermatomycosis.Therefore, the main goals of pathogenetic therapy are the improvement of microcirculation in the distal parts of the extremities, venous outflow of the extremities, normalization of the level of thyrostimulating hormones in patients with thyroid gland diseases, carbohydrate metabolism in patients with diabetes, etc.pituitary-hypothalamus-gonad system.This leads to circulatory disorders in the distal extremities, microcirculation disorders and peripheral innervation.A set of measures to correct these disorders includes acupuncture, transcranial electrical stimulation of the subcortical centers of the brain and prescription of drugs that correct the work of the sympathetic and parasympathetic autonomic nervous system.All this enables a faster clinical effect in the treatment of dermatomycosis.It is recommended to prescribe pathogenetic therapy in patients with dermatomycosis with underlying diseases before starting etiotropic treatment and to continue it throughout the duration of taking antifungal drugs.
Symptomatic therapydermatomycosis, the aim of which is to reduce subjective complaints of patients and objective manifestations of the disease, cannot replace etiotropic therapy.However, its use in combination with antifungal drugs allows for rapid improvement of the patient's condition, reduction of discomfort and elimination of cosmetic defects.In onychomycosis, the biggest concern for patients is caused by deformed, significantly thickened (hypertrophied) nail plates - onychogryphosis.Hardware pedicure is used to correct this condition.The device, which resembles a dental turbine, mechanically removes changed areas of the nails, hyperkeratotic areas, horny masses from the skin, calluses in a short period of time.In this case, there is no trauma to the nail matrix, and the patient remains functional after the procedure.
For limited nail damage (no more than 3 nail plates and no more than 1/2 of the surface from the distal edge) local preparations are used.It is recommended to start the treatment by cleaning the affected area of the nail plate with hardware pedicure or keratolytic agents.Antifungal drugs are then applied to the affected nail plate.Amorolfine solution containing ciclopirox is applied to the nail plate 1-2 times a week.Before applying the varnish, you do not need to clean the nail plate from the previous layers of preparations.The nail polish is applied daily until the healthy nail plate has completely grown.On the seventh day, the nail plate is cleaned with any cosmetic product for removing nail polish.There are conflicting reports in the literature about the effectiveness of this treatment method.The percentage of cure for patients is indicated from 5-9 to 50%.
In case of widespread damage to the nail plates of the fingers, the complex of treatment measures should include the prescription of a systemic antimycotic, nail cleaning and external therapy with antifungal drugs.In order to prevent re-infection, it is necessary to treat the patient's gloves and disinfect personal hygiene items (cloths, towels, nail files, graters and scrapers for treating skin and nails).
The drug of choice for the treatment of onychomycosis of any location is terbinafine.It is prescribed to adults and children weighing over 10 kg, 250 mg per day for 6 weeks.Children older than 2 years and weighing less than 20 kg are prescribed terbinafine in a dose of 67.5 mg/kg per day, from 20 to 40 kg - 125 mg/kg per day for 6 weeks.Backup drugs are products containing itraconazole and fluconazole.Itraconazole is administered in two regimens: 200 mg daily for 3 months or 200 mg twice daily for 7 days in the first and fifth weeks from the start of therapy.Itraconazole is not prescribed for the treatment of onychomycosis in children.Fluconazole is recommended to be taken at 150 mg once a week for 3-6 months.
Implementation of complex therapy, which consists of taking a systemic antimycotic, nail cleaning, local use of antifungal drugs, as well as antiepidemiological measures, ensures high efficiency in the treatment of foot onychomycosis.Terbinafine is prescribed for adults and children weighing more than 10 kg, 250 mg per day for 12 weeks or more.For children older than 2 years, whose weight is less than 20 kg, the drug is prescribed in a dose of 67.5 mg/kg per day, from 20 to 40 kg - 125 mg/kg per day for 12 weeks.It is recommended to use fluconazole at a dose of 150-300 mg once a week for 6-12 months.Itraconazole is used in two regimens: 200 mg daily for 3 months or 200 mg twice daily for 7 days in the first, fifth, and ninth weeks.If the big toes are affected, it is recommended to carry out the 4th course of pulse therapy in the thirteenth week from the beginning of the therapy.Itraconazole is not used to treat onychomycosis in children.
The criterion for mycological cure of onychomycosis is negative results of microscopic and cultural examination of the nail plate.After treatment with itraconazole and terbinafine, healthy nail plates do not grow completely, so a complete clinical recovery can be observed only 2-4 months after stopping the use of antifungal drugs.
















